Calf immunity #1 – What is it and how do we optimize it in the preweaned calf?
*Post contributed by Julia Hamann, D.V.M., Field Technical Specialist Diamond V
We are pleased to present a three part series on how to optimize immunity in the preweaned calf contributed by Dr. Julia Hamann, Field Technical Services Veterinary Specialist for Diamond V. We will post these over the next month under the CALF MANAGEMENT banner on the blog and CALF HEALTH section. This is great reading as it describes the biology of immunity, the role of colostrum and development of the GI tract in the calf and how to optimize immunity in this young calf.
Calf immunity #1 – The three components of immunity in the calf.
Calf immunity #2 – Colostrum and the calf’s gastrointestinal development
Calf immunity #3 – Optimizing absorption and achieving the benefits of colostrum.
The proper response of the immune system is a critical part for the animal health. There are 3 components of the immune system:
- Barrier –Skin, mucosal epithelium the lining the gut and respiratory tract (Fire Wall), and secretions (tears saliva, acidic secretions, urine, etc.)
- The immune defense against most undesirable microorganisms starts with these barriers. This comprises the calf’s first line of defense.
- Innate immune response
- If this first line of defense fails, this response will be activated, with phagocytic cell, cytokines, and proteins, attacking the invasive organisms.
- It does not need prior exposure to antigen (foreign substance which induces an immune response), and it does not have memory.
- Another function of the innate response is to activate the adaptive or acquired immune response.
- Adaptive Immune response
- This response develops more slowly,
- Immunity is antigen-specific, and it has memory. This means the body responds specifically to the disease-causing agent and can respond rather quickly.
The main goal of the immune system is to keep the animal healthy, ensuring homeostasis (the stable regulation of the animal immune response). Homeostasis = health.
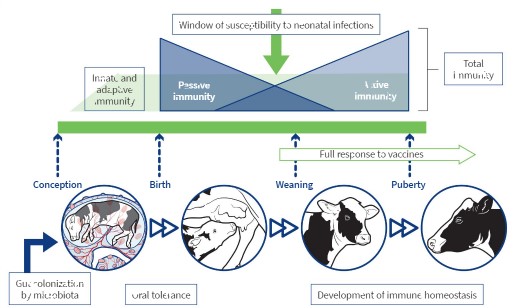
The calf is born with all the components of its immune system, but it is immunological naïve. It has not yet been exposed to antigens.
![]()
Due the nature of the cow placenta, the calf does not obtain the maternal antibodies until the intake of colostrum. The enteric passive transfer of maternal antibodies and cells during the ingestion of colostrum will provide the calf with immunological protection during a least the first 2-4 weeks of life. We must maintain high sanitary standards to secure the transfer of colostral cells and antibodies and avoid Failure Passive Transfers (FPT in newborn calves is defined as IgG concentrations in serum levels less than 10 g/l 24 to 48 hours after birth). All calves should receive colostrum containing 50 to 75 g/L of IgG to ensure a successful passive transfer. Calves that experience FPT are more likely to become sick or die from intestinal, respiratory or systemic diseases. Sadly, FPT occurring a least one calf in 41% of dairy calf operations in the USA (Beam et al., 2009).
Passive immunity in calves is evaluated by measuring serum or plasma IgG or serum total protein within the first 7 d of age. These measurements give us an idea of circulating concentrations of this important protein, they are also a good picture when evaluating all the additional benefits of colostral ingestion.
Consensus serum IgG concentrations and equivalent total protein (TP) and Brix measurements, and percentage of calves recommended in each transfer of passive immunity (TPI) category
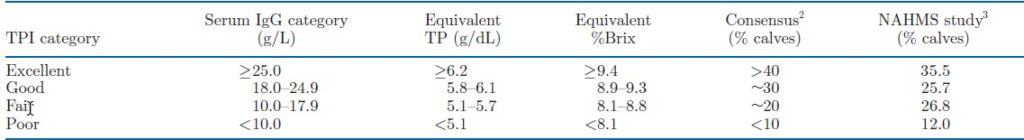
Lombard et al., 2020
Note that we used to assume that achieving a serum IgG content above 10 g/L was satisfactory. Examination of results from many calves across North America has provided us with a better tool for evaluating the success (or failure) of our colostrum management program.

Покупка 3D принтера по металлу: важные моменты
3д принтер металлом цена https://www.met3f-int43.ru .
Ensure a Stress-Free Trip
Solar Generators for RVs: A Complete Buyer’s Guide
best solar generator for rv air conditioner https://ghkolp-56dert.ru .
Stay Powered Up
Portable and Efficient: The Best Solar Generators for Home Backup
solar home backup generator http://olargener-ackup.com/ .